Ulcerative Colitis- Overview
Ulcerative Colitis is a form of inflammatory bowel disease which causes inflammation and sores in the digestive tract. It affects the innermost lining of the intestine and rectum. The symptoms develop gradually rather than suddenly.
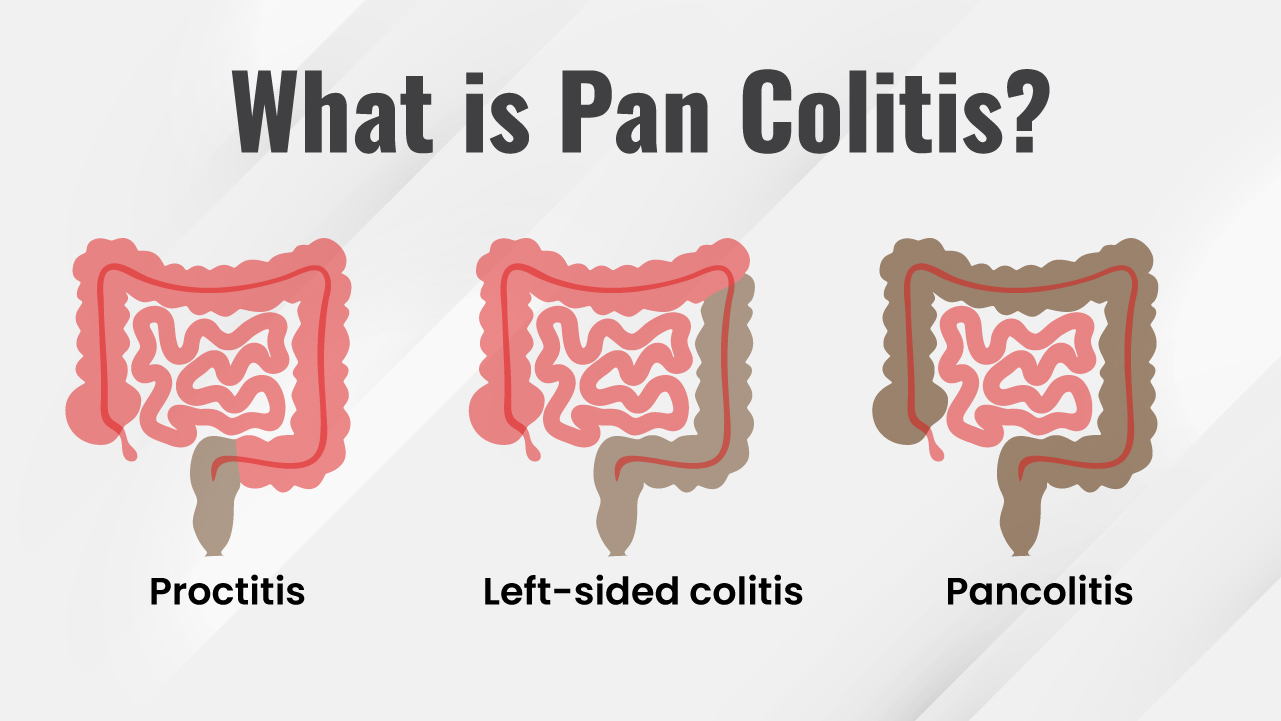
What is Pan Ulcerative Colitis or Pancolitis?
Pancolitis is a form of Ulcerative Colitis, which affects the entire large intestine. It is also known as total colitis or universal colitis. It is caused by complications of a toxic diet and lifestyle and may also be affected by infections like C.difficile. It is also associated with inflammatory disorders like rheumatoid arthritis. It develops over a long period.
Generally, pancolitis starts as a form of ulcerative colitis in the rectum. Over time, the inflammation extends to the surrounding tissues too, and slowly the entire colon is affected. This condition is pancolitis.
Unfortunately, there is no known cure for pancolitis, but the condition can be reversed if diet and lifestyle are addressed.
Other types of ulcerative colitis are:
- Proctosigmoiditis
- Proctitis
- Left-Sided or distal Ulcerative Colitis
As more parts of the colon get affected, the chances of symptoms getting more painful and uncomfortable increase. As pancolitis affects the whole colon, the symptoms can get worse than the other forms.
Causes of Pan Ulcerative Colitis or Pancolitis
The exact cause of pancolitis is still unknown. As with other inflammatory bowel diseases, pancolitis can be caused by genes. The environment also plays an important role. Anti-inflammatory drugs or other sorts of medication can also increase the risk. One of the most common factors is a high-fat diet. Other factors include:
- Genetic predisposition
- Abnormal reaction from the digestive system to intestine bacteria
- Abnormal immune response
- Unknown triggers (virus, bacteria, stress, or diet)
In certain cases, when a person doesn’t get treatment for mild forms of UC, the condition can worsen and result in pancolitis. Around 20% of people who have ulcerative colitis will have pancolitis. It is also believed that stress and anxiety can lead to UC and pancolitis. Stress and anxiety can trigger ulcers, causing pain and discomfort. But these factors don’t actually cause pancolitis.
Symptoms of Pan Ulcerative Colitis or Pancolitis?
Common symptoms of pancolitis include:
- Feeling Exhausted
- Abnormal Weight Loss
- Abdomen pain and cramps
- Frequent urge for bowel movement
The above-mentioned symptoms are common in the mild and moderate stages of pancolitis. As the pancolitis gets severe, you will likely have symptoms like:
- Pain and bleeding in the rectum and anal area
- Unexplained fever
- Diarrhea with blood
The growth of children can be compromised if they suffer from pancolitis.
Sometimes these symptoms may not necessarily be pancolitis. Cramp, pain, nausea, and a strong urge to pass waste can also be caused by food poisoning, gas, or bloating. In these cases, the symptoms will go away after a short period.
Other Complications
The severity of symptoms can vary and affect the digestive system, and the cause is still unknown, although we know that diet and lifestyle play a big role. While some people are affected for a long period with low and mild symptoms, few people face the effects significantly throughout their lives. Other complications that might arise when the condition gets severe include the following:
- Cancer:
Pancolitis patients have a greater chance of developing bowel cancer when they have been suffering from it for years.
- Toxic Megacolon:
The colon can acutely dilate when the inflammation becomes severe, which is also known as toxic megacolon. The symptoms are much similar, which includes fever, abdominal pain, dehydration, and malnutrition. Toxic megacolon also increases the risk of colonic rupture.
- Anaemia:
Anaemia is commonly caused due to the inability of inflamed intestines to absorb nutrients. It can be treated with iron-rich food consumption.
- Fulminant Colitis:
It is quite rare but can happen in case of severe pancolitis. Patients reach this level due to dehydration, severe abdominal pain, and diarrhea with bleeding. This also increases the risk of developing toxic megacolon or colonic rupture.
Remedies for Pan Ulcerative Colitis
Pancolitis treatment depends on how severe the condition is and how much the symptoms affect the person’s life. There is no known cure, thus the aim remains towards reducing the symptoms until they are gone. For a person with UC, many can find symptom relief by making simple lifestyle changes. Dietary changes make a huge difference in reducing symptoms and flare-ups. Some easy remedies include:
- Drinking plenty of water
- Increasing calcium and vitamin D in the diet
- Eating small meals rather than large ones at a go
- Reducing consumption of greasy & buttery foods
- Avoiding milk products
Other than dietary changes, the following changes might prove fruitful:
- Get Regular Exercise to Reduce UC Inflammation
- Stress Less to Aid Digestion Problems in UC
- Consider Therapy to Help Manage Stress and Pain
- Experiment With Herbal Remedies for Ulcerative Colitis
Conclusion:
Pancolitis causes inflammation in the entire colon and although it is different and possibly more painful than Ulcerative colitis, it can be healed with natural methods like dietary and lifestyle changes. A whole food plant-based diet helps tackle the root of the issue and recover from pan ulcerative colitis.
FAQ
- What is severe pancolitis?
Pancolitis is an inflammation of the entire colon, which is a common cause of ulcerative colitis. It can be caused by complications of a toxic diet and lifestyle and may also be affected by infections like C. difficile or inflammatory disorders like rheumatoid arthritis.
- Can Pancolitis be life-threatening?
It is a chronic condition without cure and patients have to live with experiencing significant physical and emotional issues. Conditions can get intense during flare-ups, but during the remission period, they can lead a normal life.
- Is pancolitis hereditary?
Hereditary is most definitely a risk factor in the development of ulcerative colitis. However, we know now due to the field of epigenetics, environmental factors play a much larger role in whether the disease will manifest. Our genes might load the gun, but our diet, lifestyle and environmental factors pull the trigger.
